A rare viral disease linked to rodent exposure has killed three people aboard a cruise ship in the Atlantic Ocean, prompting questions about hantavirus and its transmission. Here is what you need to know.
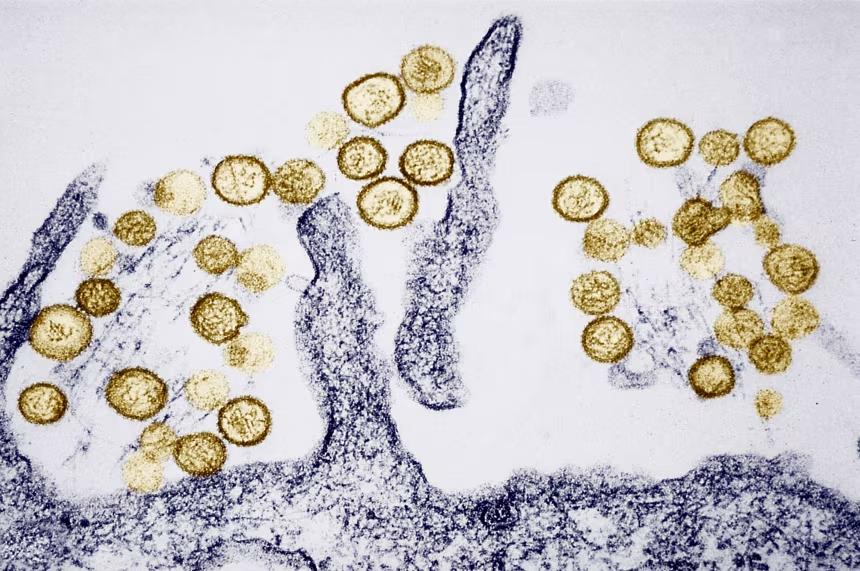
What is hantavirus?
Hantavirus refers to a group of viruses spread by rodents through their urine, droppings and saliva. The virus is named after the Hantaan River in South Korea, where it was first identified in the 1970s.

Humans typically become infected when they inhale airborne particles from dried rodent droppings. This often happens when someone sweeps up rodent waste, causing contaminated dust to become airborne. People can also contract the virus by touching contaminated surfaces and then touching their mouth or nose, or through rodent bites, though this is rare.
The most concerning aspect of the current outbreak is that human-to-human transmission cannot be ruled out. Dr Maria Van Kerhove, the World Health Organisation’s Director for Epidemic and Pandemic Preparedness and Prevention, confirmed that some cases had very close contact with each other, making person-to-person spread a possibility.
Only one hantavirus strain, the Andes virus native to South America, has been documented spreading between humans, and this remains extremely rare.
What are the symptoms?
Hantavirus causes two distinct types of severe illness, depending on where the virus originates.
In Europe and Asia, the virus causes haemorrhagic fever with renal syndrome, which affects the kidneys. Initial symptoms include headaches, abdominal pain and nausea. The disease can progress to low blood pressure, internal bleeding and acute kidney failure. Between five and 15 per cent of cases are fatal, according to the United States Centers for Disease Control and Prevention. Symptoms typically develop one to two weeks after exposure.
In the Americas, hantavirus causes hantavirus pulmonary syndrome, which affects the lungs. The illness begins with flu-like symptoms including fatigue, fever, chills and body aches. Over time, patients may experience severe shortness of breath and chest tightness as fluid fills the lungs. Symptoms can take one to eight weeks to develop after exposure. Nearly 40 per cent of those who develop respiratory symptoms may die from the disease.
Is there a cure?
No specific treatment exists for hantavirus infection. Patients receive supportive care including hydration, rest and symptom management. For severe cases affecting the lungs or kidneys, intensive care may be required.
The lack of a cure makes prevention critical. The CDC recommends keeping rodents out of homes by sealing gaps and holes, storing food in secure containers, and disposing of rubbish in thick bins with tight lids.
When cleaning rodent droppings, wear gloves, spray the waste with a bleach solution, wait five minutes, then wipe with paper towels and dispose of them safely. Never sweep or vacuum rodent droppings dry, as this releases infectious particles into the air.
How common is hantavirus?
Globally, between 60,000 and 100,000 cases of haemorrhagic fever with renal syndrome occur each year, with China accounting for roughly half of all cases, according to a 2024 study.
In the United States, 890 cases were reported between 1993 and 2023, most occurring in western states.
The disease gained attention in 2025 after Betsy Arakawa, wife of Oscar-winning actor Gene Hackman, died from hantavirus pulmonary syndrome at age 65. Public health records revealed dead rodents and nests throughout outbuildings on the couple’s property in New Mexico.
How did the cruise ship outbreak occur?

The source of infection remains under investigation. The WHO confirmed seven cases, including two laboratory-confirmed infections and five suspected cases, following an outbreak on a cruise ship travelling from Argentina to Cape Verde.
Dr Charlotte Hammer, an epidemiologist at the University of Cambridge, said several scenarios are possible. Rodents could have boarded the ship, or passengers may have been infected during the ship’s last port stop in Argentina. Given hantavirus has an incubation period of one to eight weeks, infection could have occurred before boarding.
Dr Scott Miscovich, president of Premier Medical Group, said thorough investigation is required. “All the droplets, all the dust in every room, all the kitchens, all the ventilation systems need to be sampled and then cultured,” he said.
The WHO is conducting detailed investigations, including genetic sequencing to determine which viral strain infected passengers.
Should Nigerians be concerned?
The WHO has assessed the risk to the global population as low. Human-to-human transmission remains extremely rare, and no cases have been reported in Nigeria.
The outbreak originated on the cruise ship, but passengers who disembarked at Saint Helena have dispersed globally. Health authorities across multiple countries are coordinating international response efforts, conducting contact tracing and monitoring returned passengers.
For Nigerians, the standard prevention measures apply: maintain clean living spaces, seal entry points where rodents could enter, store food properly, and use safe cleaning methods if rodent droppings are discovered.
The establishment of the International Media and Information Literacy Institute in Abuja last week underscores Nigeria’s commitment to combating misinformation during health emergencies. Accurate, verified information remains the best defence against panic.